
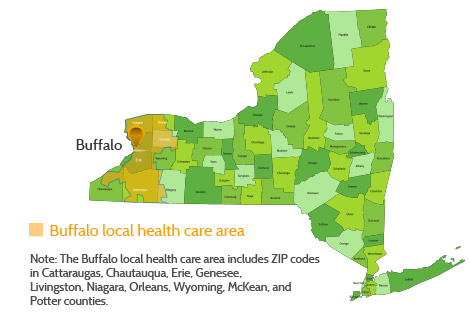
 Leaders in Buffalo and other parts of Western New York have been working to reverse decades of economic decline that began in the 1950s, soon after the St. Lawrence Seaway opened, diverting shipping traffic away from the area. The region's troubles continued into the 1970s and 1980s as its steel industry contracted and manufacturing jobs moved overseas. Efforts to recruit businesses in new industries and revitalize older ones have emphasized enhancing the region's reputation for delivering high-quality, complex care (to keep local patients from traveling outside the region and to attract others from nearby states) and improving the health of the population to further lower health care costs, which are already below national norms.
Leaders in Buffalo and other parts of Western New York have been working to reverse decades of economic decline that began in the 1950s, soon after the St. Lawrence Seaway opened, diverting shipping traffic away from the area. The region's troubles continued into the 1970s and 1980s as its steel industry contracted and manufacturing jobs moved overseas. Efforts to recruit businesses in new industries and revitalize older ones have emphasized enhancing the region's reputation for delivering high-quality, complex care (to keep local patients from traveling outside the region and to attract others from nearby states) and improving the health of the population to further lower health care costs, which are already below national norms.
Strong social ties–stemming from a distinct pride of place and the reliance on one's neighbors–have facilitated these efforts, says Michael Cropp, M.D., president and CEO of Independent Health, one of several payers that partner with local providers to prioritize areas of focus and agree on common measures, thereby amplifying the impact of quality improvement and pay-for-performance programs.

Investments in a regional health information exchange known as HEALTHeLINK have also increased efficiency by enabling the sharing of clinical and administrative data among hospitals, physicians, and insurers. This wouldn't have been possible without coordinated action. "There are some forward-thinking folks here in our community that got together from the major health plans and hospitals and said 'We could either do this in a collaborative manner or we can do it separately, but it's something that we all have to invest in,'" says Daniel E. Porreca, HEALTHeLINK's executive director.

Support from foundations has also been key. "Improving outcomes and reducing costs really requires a commitment to capacity building in the community," says Ann Monroe, president of Health Foundation for Western & Central New York, which along with the John R. Oishei Foundation has devoted substantial resources to encouraging the collaborative effort to improve care in Western New York. In one example, foundation money has supported safety-net providers coming together for mutual support and to identify areas in need of expanded services, which may drive further efficiencies.


KC Kratt

KC Kratt
KC Kratt
Acknowledgments
The case studies were developed as part of a grant from The Commonwealth Fund to the Institute for Healthcare Improvement (IHI). The authors are grateful to the many individuals who shared perspectives on the case study regions and on regional health system performance. We acknowledge the support of our colleagues at The Commonwealth Fund and our coauthor, Sandy Cohen, at IHI.
The views presented here are those of the authors and not necessarily those of the Institute for Healthcare Improvement or The Commonwealth Fund or their directors, officers, or staff. These case studies were based on publicly available information and self-reported data provided by the case study participants. The Commonwealth Fund is not an accreditor of health care organizations or systems, and the inclusion of an institution in the Fund’s case study series is not an endorsement by the Fund for receipt of health care from the institution.
