Aiming Higher: Results from the Commonwealth Fund Scorecard on State Health System Performance
Highlights from the Scorecard
The 2017 edition of the Commonwealth Fund Scorecard on State Health System Performance finds that nearly all state health systems improved on a broad array of health indicators between 2013 and 2015. During this period, which coincides with implementation of the Affordable Care Act’s major coverage expansions, uninsured rates dropped and more people were able to access needed care, particularly those in states that expanded their Medicaid programs. On a less positive note, between 2011–12 and 2013–14, premature death rates rose slightly following a long decline. The Scorecard points to a constant give-and-take in efforts to improve health and health care, reminding us that there is still more to be done.
Vermont was the top-ranked state overall in this year’s Scorecard, followed by Minnesota, Hawaii, Rhode Island, and Massachusetts (Exhibit 1). California, Colorado, Kentucky, New York, and Washington made the biggest jumps in ranking, with New York moving into the top-performing group for the first time. Kentucky also stood out for having improved on more measures than any other state.
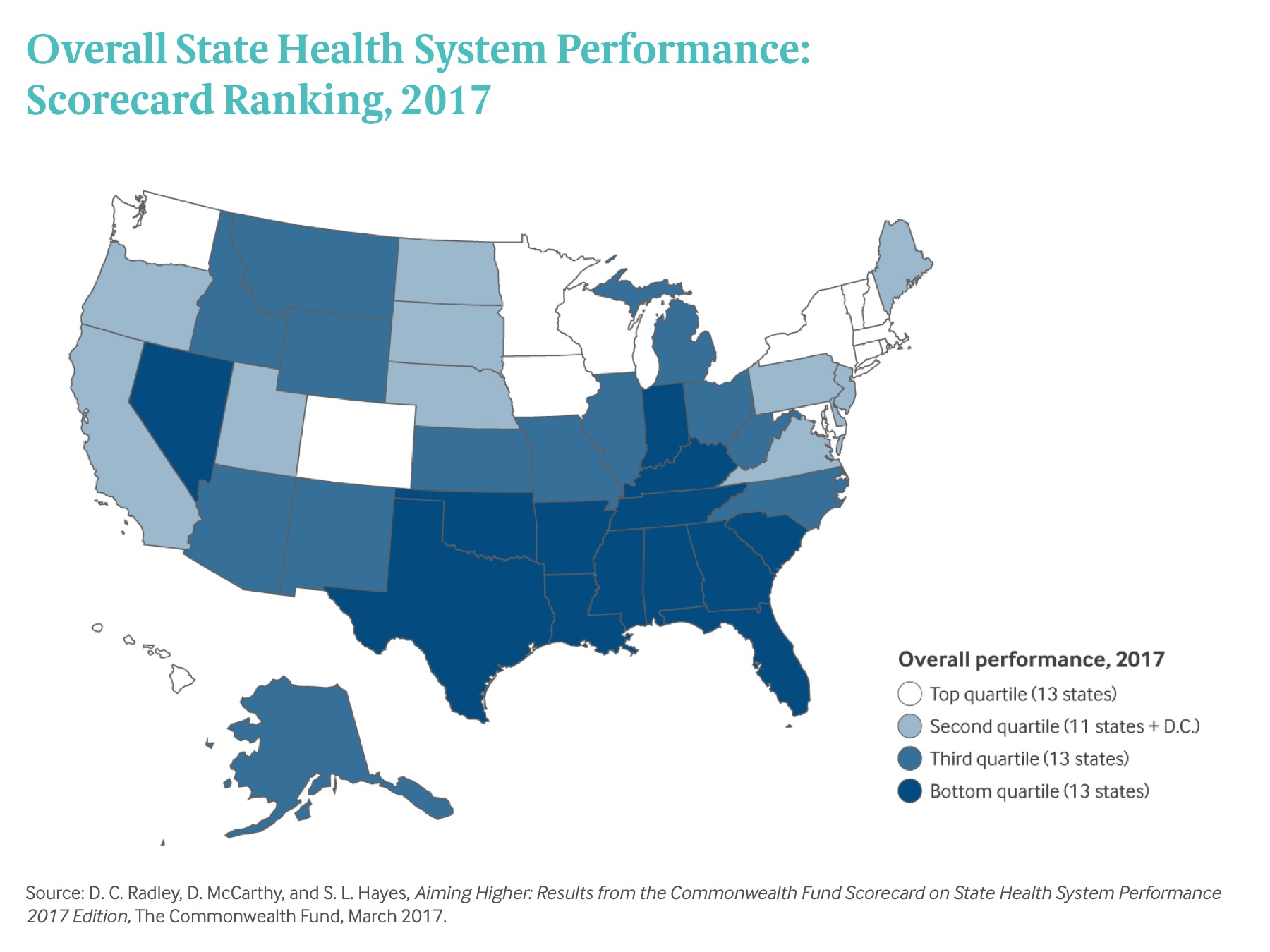
Using the most recent data available, the Scorecard ranks states on more than 40 measures of health system performance in five broad areas: health care access, quality, avoidable hospital use and costs, health outcomes, and health care equity. In reviewing the data, four key themes emerged:
- There was more improvement than decline in states’ health system performance.
- States that expanded Medicaid saw greater gains in access to care.
- Premature death rates crept up in almost two-thirds of states.
- Across all measures, there was a threefold variation in performance, on average, between top- and bottom-performing states, signifying opportunities for improvement.
By 2015, fewer people in every state lacked health insurance. Across the country, more patients benefited from better quality of care in doctors’ offices and hospitals, and Medicare beneficiaries were less frequently readmitted to the hospital. The most pervasive improvements in health system performance occurred where policymakers and health system leaders created programs, incentives, or collaborations to ensure access to care and improve the quality and efficiency of care. For example, the decline in hospital readmissions accelerated after the federal government began levying financial penalties on hospitals that had high rates of readmissions and created hospital improvement innovation networks to help spread best practices. (notes) R. B. Zuckerman, S. H. Sheingold, E. J. Orav et al., “Readmissions, Observation, and the Hospital Readmissions Reduction Program,” New England Journal of Medicine, April 21, 2016, 374(16):1543–51; R. A. Berenson and T. Rice, “Beyond Measurement and Reward: Methods of Motivating Quality Improvement and Accountability,” Health Services Research, Dec. 2015, 50(Suppl. 2):2155–86; Centers for Medicare and Medicaid Services, Partnership for Patients.
Still, wide performance variation across states, as well as persistent disparities by race and economic status within states, are clear signals that our nation is a long way from offering everyone an equal opportunity for a long, healthy, and productive life. Looking forward, it is likely that states will be challenged to provide leadership on health policy as the federal government considers a new relationship with states in public financing of health care. To improve the health of their residents, states must find creative ways of addressing the causes of rising mortality rates while also working to strengthen primary and preventive care.
(See Methods and Appendix for a complete description of how the Scorecard was developed and detail on indicators and measurement periods.)
More Improvement than Decline in States’ Health System Performance
Health system performance improved in more instances than it worsened from 2013 to 2015, (notes) The Scorecard evaluates change for 39 of the 44 performance indicators for which data were available over time. Performance measures are constructed from the most recently available data, generally reflecting the two-year period ending in 2014 or 2015, though this does vary somewhat by indicator. We identified instances of improvement or worsening that can be considered meaningful if there was at least 0.5 standard deviation change between the indicators’ observed rates in the two periods. Refer to report appendix for more detail on performance measures included here. reversing states’ performance trajectory coming out of the recession of 2007–09. (notes) D. C. Radley, D. McCarthy, J. A. Lippa, S. L. Hayes, and C. Schoen, Aiming Higher: Results from a Scorecard on State Health System Performance, 2014 (The Commonwealth Fund, May 2014) All but four states (Alaska, Hawaii, New Hampshire, Oregon) improved on at least twice as many indicators as they worsened on. Kentucky and Oklahoma were “most improved”— meeting or exceeding the Scorecard’s threshold for improvement on 21 and 19 indicators respectively. All states and the District of Columbia worsened on at least one indicator.
Widespread and Unprecedented Gains in Access
Health System improvement over time is not a given. As documented previously in our Scorecard series, worsening or stagnating performance was pervasive across states in the first decade of the 2000s, particularly on indicators of health care access, as the number of uninsured adults continued to rise and more people skipped needed care. (notes) D. C. Radley, D. McCarthy, J. A. Lippa, S. L. Hayes, and C. Schoen, Aiming Higher: Results from a Scorecard on State Health System Performance, 2014 (The Commonwealth Fund, May 2014); D. McCarthy, S. K. H. How, C. Schoen, J. C. Cantor, D. Belloff, Aiming Higher Results from a State Scorecard on Health System Performance, 2009 (The Commonwealth Fund, October 2009).
The implementation of the Affordable Care Act’s major coverage expansions in 2014 led to a sharp reversal in these access trends. In this year’s Scorecard, these expansions were associated with improvements on at least three indicators of access to care in the majority of states. Between 2013 and 2015, nearly all states and the District of Columbia met the Scorecard’s threshold for improvement of at least a three-percentage-point decline in the uninsured rate for adults ages 19 to 64. More than half of states improved—at least a two-point reduction— in their uninsured rate for children. Three-quarters of states and the District of Columbia had a drop of at least two percentage points in the share of adults (age 18 and older) who reported not going to the doctor when they needed to because of costs (Exhibit 3).
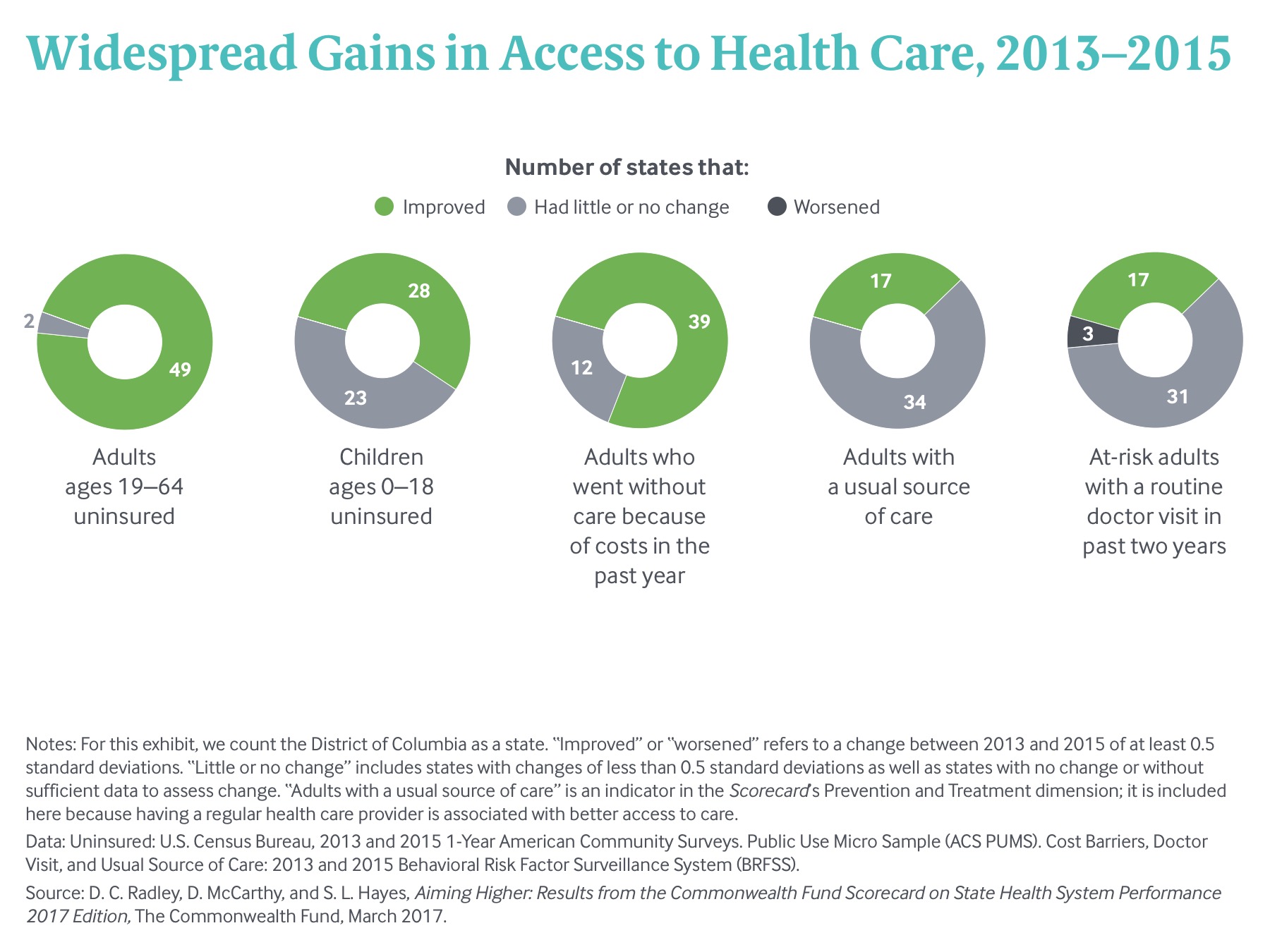
Research has shown that people with health insurance coverage are more likely than those without to have a usual source of care and to have had a recent health care visit. (notes) Centers for Disease Control/National Center for Health Statistics, “Health Insurance and Access to Care,” National Center for Health Statistics Fact Sheet, Nov. 2015. In the first two years of the coverage expansions, about a third of states, along with the District of Columbia, saw jumps in the share of adults with a usual doctor or health care provider and in the share of “at risk” adults with a routine check-up in the past two years (Exhibit 3). At-risk adults are those age 50 or older, as well as younger adults with a chronic illness or in fair or poor health.
Read more about health care access across states.
Improvements Aided by Targeted Reforms
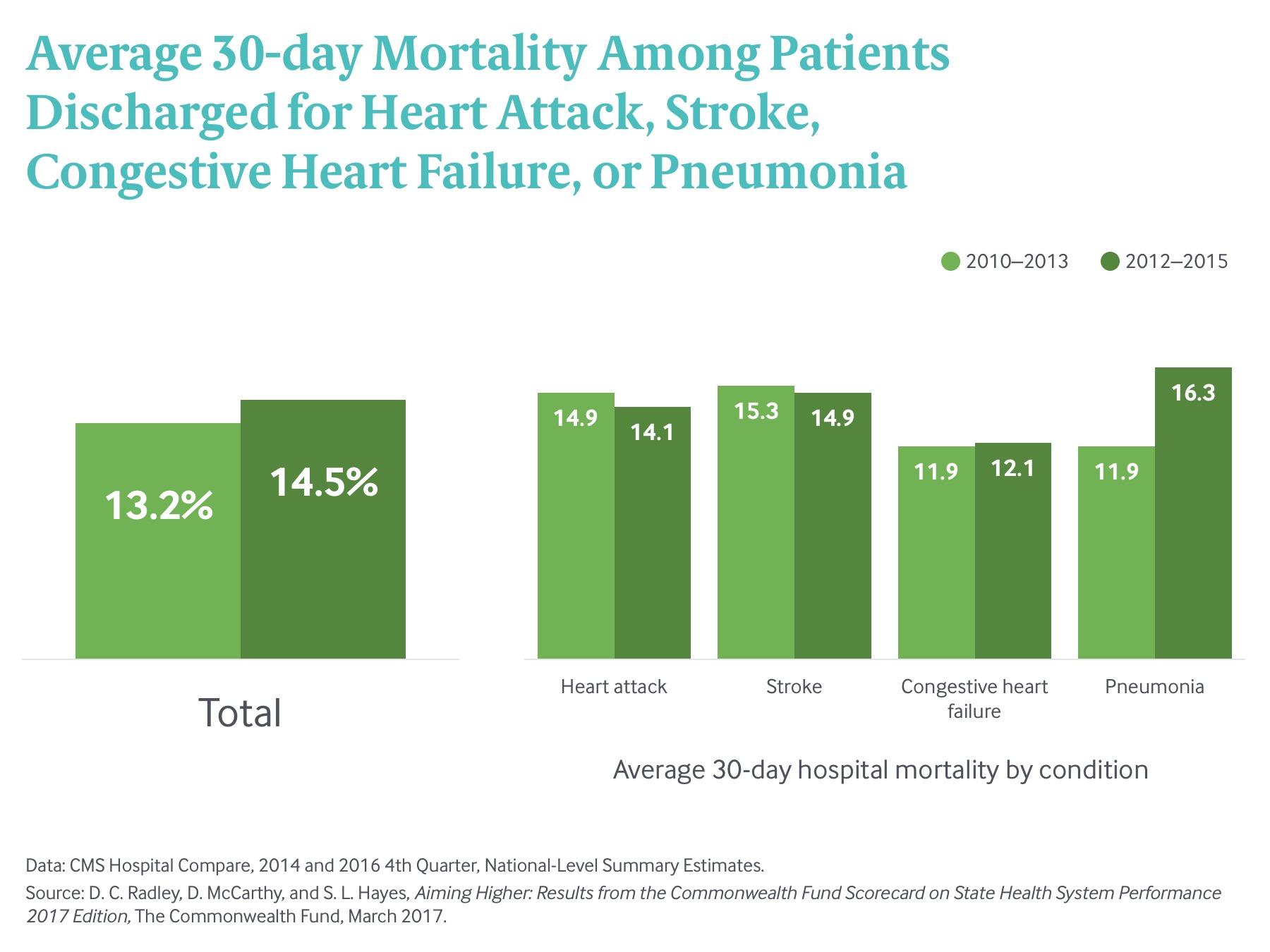
States made progress in other areas that were the target of concerted efforts to improve health system performance. For example, the Hospital Readmission Reduction Program, established by the Affordable Care Act, requires the Centers for Medicare and Medicaid Services (CMS) to reduce reimbursement to hospitals that have higher-than-expected readmissions of Medicare beneficiaries discharged from the hospital in the previous 30 days after being treated for certain conditions. The payment penalties began in October 2012; between 2012 and 2014, 33 states and the District of Columbia substantially lowered their all-cause readmission rate among Medicare beneficiaries. The largest reductions of 12 to 13 readmissions per 1,000 Medicare beneficiaries were in Kentucky, Illinois, and D.C., all of which had the highest rates at the outset (Exhibit 4).
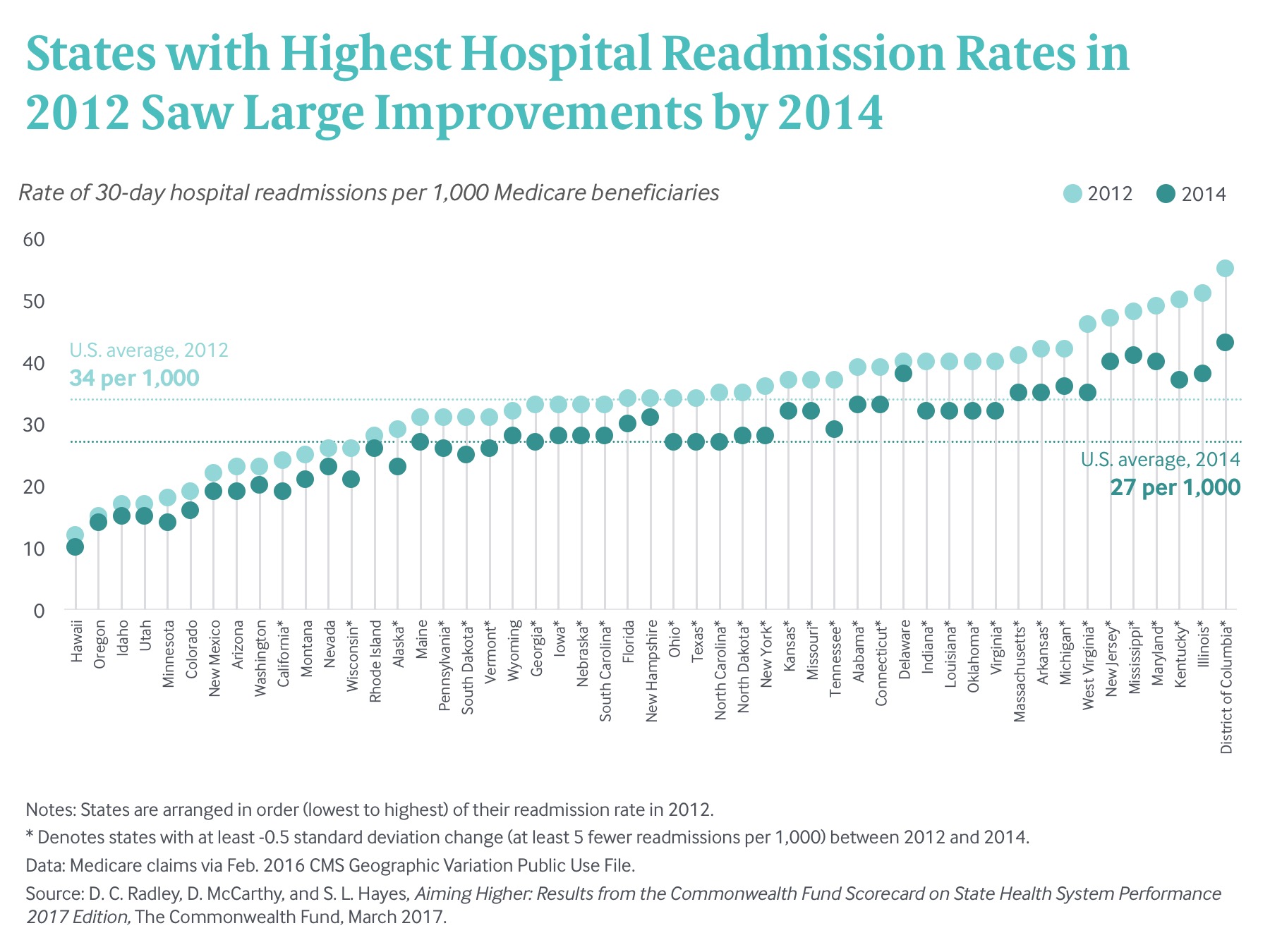
Public policies and private partnerships have also focused on improving patient safety across care settings. In recent years, there has been growing uptake of electronic prescribing and associated clinical decision support, aggressively encouraged by the federal government through incentives for implementing electronic health records. (notes) M. H. Gabriel and M. Swain, “E-Prescribing Trends in the United States,” ONC Data Brief, No. 18 (Office of the National Coordinator for Health Information Technology, July 2014); A. Porterfield, K. Engelbert, and A. Coustasse, “Electronic Prescribing: Improving the Efficiency and Accuracy of Prescribing in the Ambulatory Care Setting,” Perspectives in Health Information Management, Spring 2014: 1–13; B. Clyne, M. C. Bradley, C. Hughes et al., “Electronic Prescribing and Other Forms of Technology to Reduce Inappropriate Medication Use and Polypharmacy in Older People: A Review of Current Evidence,” Clinics in Geriatric Medicine, May 2012 28(2):301–22. This change may explain in part why Medicare beneficiaries in 46 states were less likely to be prescribed a high-risk medicine in 2014 than in 2012. In hospitals, progress is being made in reducing costly and potentially deadly central line-associated bloodstream infections (CLABSIs), as strategies for reducing their incidence are refined and implemented more widely. For the first time, the Scorecard can track state-level average CLABSI rates; it found notable declines relative to a national benchmark between 2013 and 2014 in 20 states and the District of Columbia (Exhibit 5).
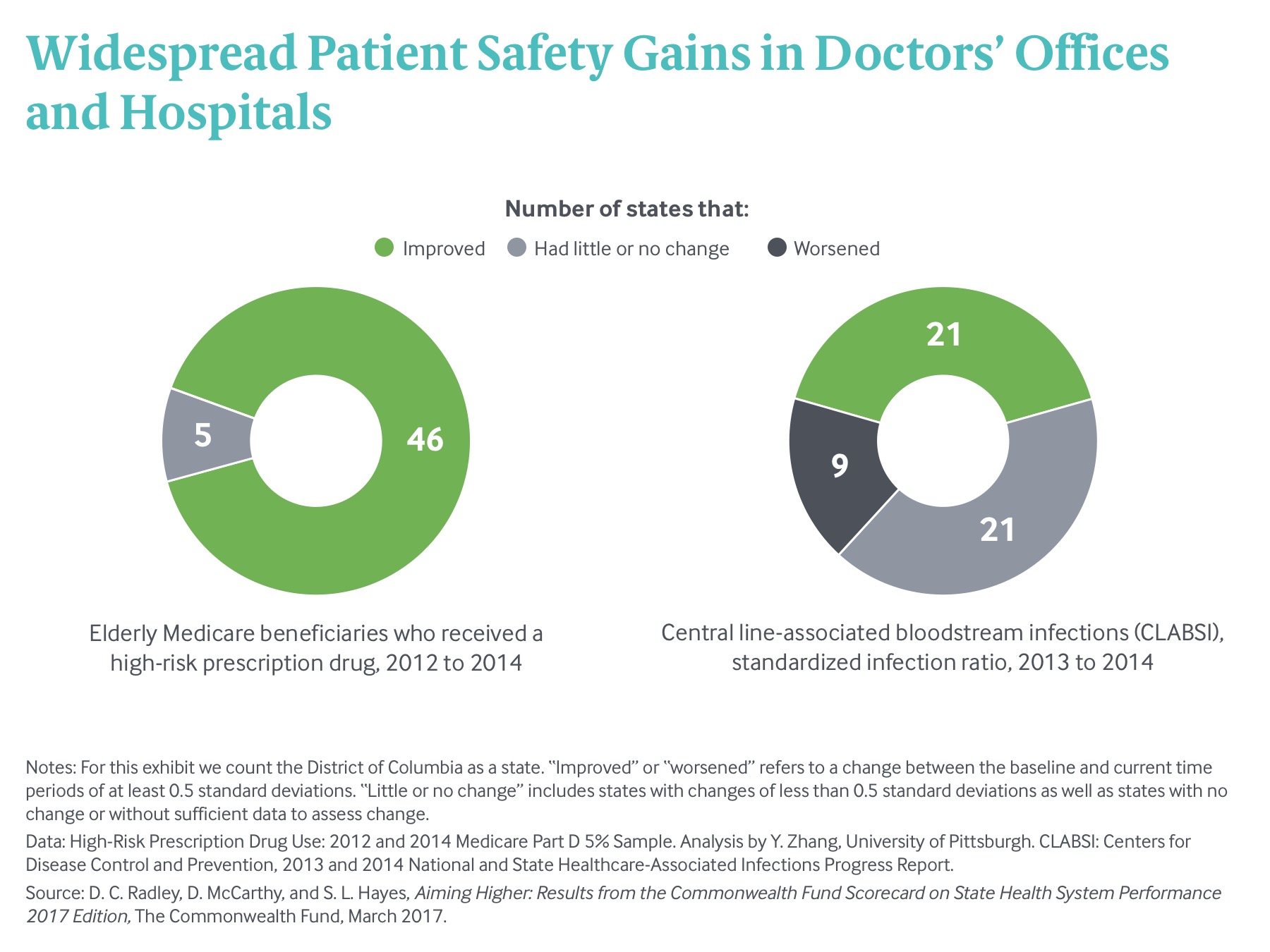
States Expanding Medicaid Saw Greater Gains in Access
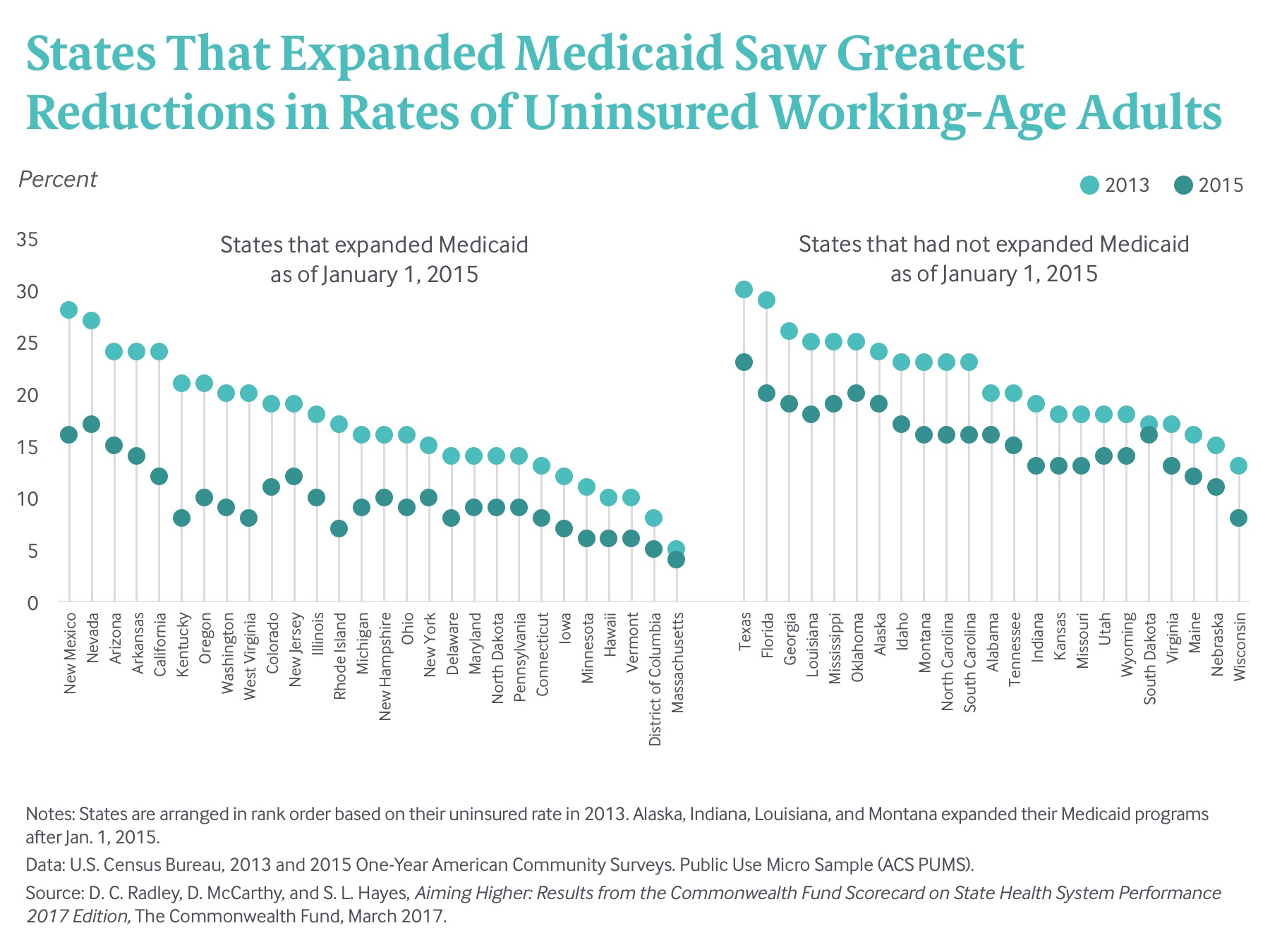
The Scorecard finds that states that accepted federal funding to expand their Medicaid programs under the Affordable Care Act outperformed states that did not expand Medicaid. (notes) The Scorecard sets January 1, 2015, as the cutoff date for which a state would be considered an expansion state, because this date best aligns with the health insurance coverage data used in this analysis from the American Community Survey. Alaska, Indiana, Louisiana, and Montana implemented Medicaid expansion between February 2015 and July 2016 but are considered nonexpanding states in this Scorecard. Expansion states typically ranked higher than nonexpansion states before and after the law’s coverage expansions (Exhibit 1), but they also saw the greatest gains in health care access between 2013 and 2015. For example, states that achieved double-digit reductions in their uninsured rate for working-age adults between 2013 to 2015—Arkansas, California, Kentucky, Nevada, New Mexico, Oregon, Rhode Island, Washington, and West Virginia—all had expanded Medicaid as soon as federal resources became available in 2014 (Exhibit 6). Over the two-year period, Kentucky, followed by Arkansas and Oregon, experienced the biggest drops in the share of adults 18 and older who reported forgoing needed care because of costs (7 points, 5 points, and 5 points, respectively) (Appendix C2).
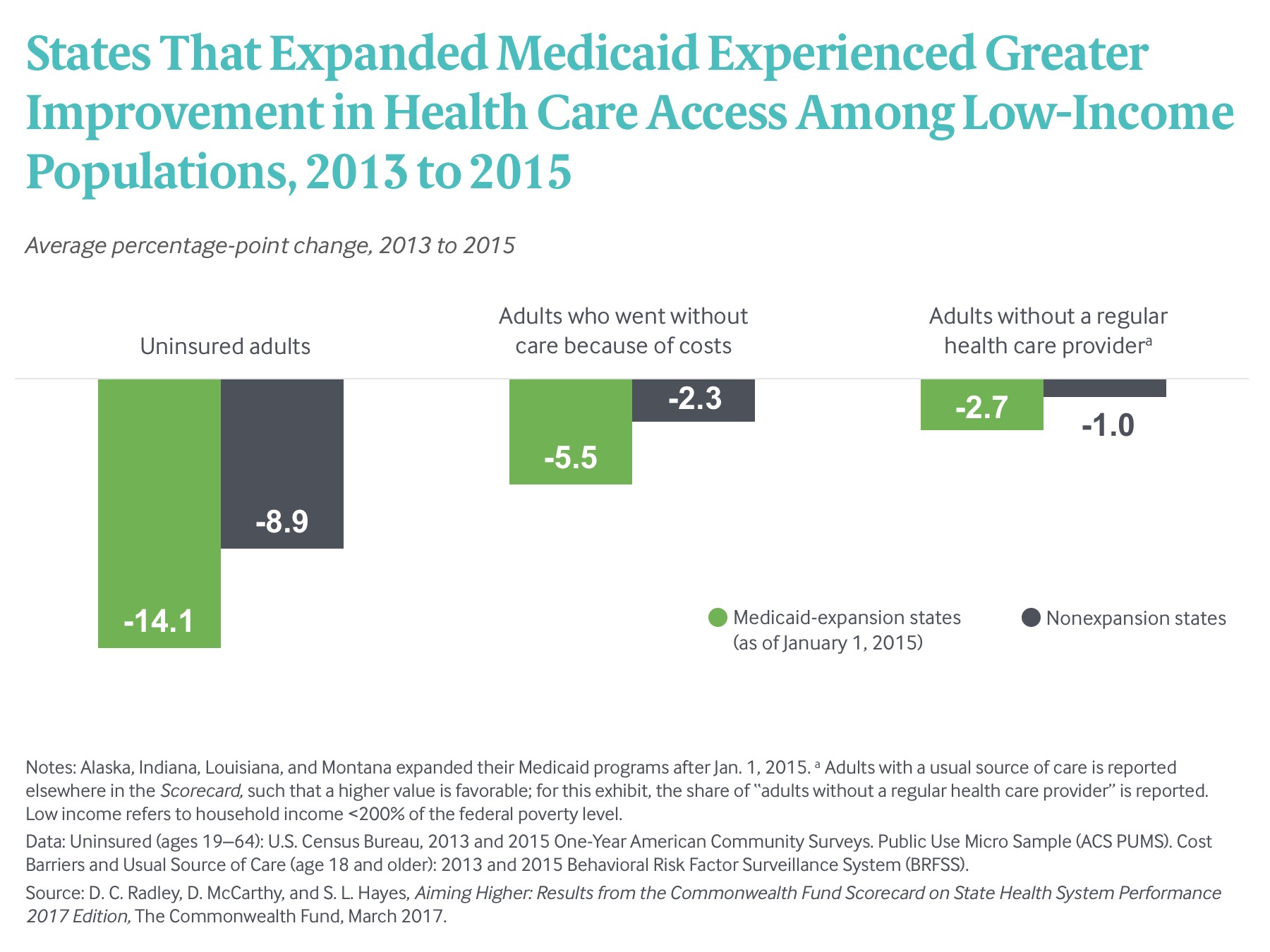
Low-income people fared relatively better in Medicaid expansion states than their counterparts did in nonexpansion states. For example, the proportion of low-income working age adults who were uninsured shrank more, on average, in states that had expanded Medicaid than in states that did not (Exhibit 7). In addition, Medicaid-expanding states saw a greater reduction in the share of low-income adults going without care because of costs or lacking a usual source of care.
The fact that nonexpansion states did not keep pace with expansion states in improving access and equity is reflected in the overall Scorecard rankings. Of the four nonexpansion states that were ranked in the top quartile of overall performance in the 2013 baseline period, only Wisconsin repeated its top quartile performance in the latest ranking (notes) Wisconsin is unique compared to other nonexpansion states in that it has higher Medicaid eligibility thresholds; for example, it provides coverage to childless adults with incomes up to 100 percent of the federal poverty level. Maine, Nebraska, and Utah all fell and dropped from the top-performance quartile.
The five states that had the most dramatic upward shifts in overall rankings were Medicaid-expansion states: California moved up 12 places; Kentucky and New York each moved up eight places; Washington jumped six spots; and Colorado rose five places.
California improved the most of any state in the 2017 overall rankings, climbing up 12 spots, from 26th place in the baseline to 14th.
California met—and in some cases far exceeded—the Scorecard’s threshold for improvement on 14 of the 39 indicators for which we had trend data. The most dramatic shifts were in uninsured rates. Between 2013, the year before the Affordable Care Act’s major coverage expansions took effect, and 2015, California sliced its uninsured rates for working-age adults and for children in half (from 24% to 12%, and 8% to 4%, respectively).
Between 2013 and 2015, the share of adults in California reporting that they went without needed care because of costs dropped by 4 percentage points, the share of adult Californians with a usual source of care jumped 6 percentage points (from 71% to 77%), and the share of at-risk adults without a recent routine doctor’s visit improved by 3 percentage points.
How did the nation’s most populous state do it? “We were ‘all in’ in terms of the ACA, and it coincided with a strong economy here in California. I’m sure the two worked off of one another,” says Chris Perrone, director of Improving Access at the California Health Care Foundation. Six months after the passage of the ACA in 2010, California became the first state to enact legislation to create its health insurance marketplace, Covered California, regarded as one of the most successful in the country. In the first three years, the average purchase price for plans on Covered California was less than the average offer price, suggesting enrollees chose lower-cost plans and prompting the authors of a research study to conclude: “Covered California demonstrates—straight out of Economics 101—if consumers have easy-to-understand, transparent information without being overwhelmed with too many choices, they will buy lower-premium products available on their tier.”
(notes)
The Commonwealth Fund, “Consumers Buy Lower-Cost Plans on Covered California, Suggesting Exposure to Premium Increases Is Less Than Commonly Reported,” In the Literature, Jan. 9, 2017. See also J. R. Gabel, D. R. Arnold, B. D. Fulton et al., “Consumers Buy Lower-Cost Plans on Covered California, Suggesting Exposure to Premium Increases Is Less Than Commonly Reported,” Health Affairs, Jan. 2017 36(1):8–15
Ibid.
California also expanded eligibility for its Medicaid program under the ACA as soon as federal resources became available in January 2014. It also devoted significant resources to outreach and enrollment efforts for both marketplace and Medicaid managed care plans.
The state improved on indicators that spanned all age groups and care settings, including a substantial decrease in 30-day hospital readmissions among Medicare beneficiaries, which at the outset was already lower than in many other states. (notes) In addition to the six indicators mentioned in the text, California improved on the following indicators: children ages 19–35 months who received all recommended doses of seven key vaccines; Medicare beneficiaries who received at least one drug that should be avoided in the elderly; Medicare beneficiaries with dementia, hip/pelvic fracture, or chronic renal failure who received a prescription drug that is contraindicated for that condition; hospitalized patients given information about what to do during their recovery at home; home health patients who get better at walking or moving around; long-stay nursing home residents with an antipsychotic medication; short-stay nursing home residents with a 30-day readmission to the hospital; and adults with poor health-related quality of life.
Premature Death Rates Crept Up in Almost Two-Thirds of States
Recent headlines point to a troubling reality in the U.S.: Americans can expect to live a shorter life than they did a decade ago.
(notes)
J.Q. Xu, S.L. Murphy, K.D. Kochanek, et al., Mortality in the United States, 2015. NCHS data brief, no. 267 (National Center for Health Statistics, 2016).
R. Stein, “Life Expectancy In U.S. Drops For First Time In Decades, Report Finds”; John Bacon “Dying younger: U.S. Life Expectancy ‘A Real Problem’,” USA Today, Dec. 8 2016.
This is primarily the result of increased deaths from heart disease and other chronic conditions. But to a lesser extent, the trend is also attributable to what Princeton economist Anne Case has called “deaths of despair”—including fatalities from opioid and alcohol abuse.
(notes)
D. Squires, “The Shortening American Lifespan,” To the Point, The Commonwealth Fund, Jan 4. 2017; A. Case, “‘Deaths of Despair’ Are Killing America’s White Working Class, Quartz, Dec. 30, 2015
Findings from the Scorecard reinforce these discouraging trends.
The Scorecard measures mortality by tracking premature death rates overall as well as by separately measuring deaths from two high-profile cancers, suicide, and infant mortality. It is important to note that mortality data reported in the Scorecard extend only through 2014, the latest year available, and include deaths that occurred before insurance coverage expansions.
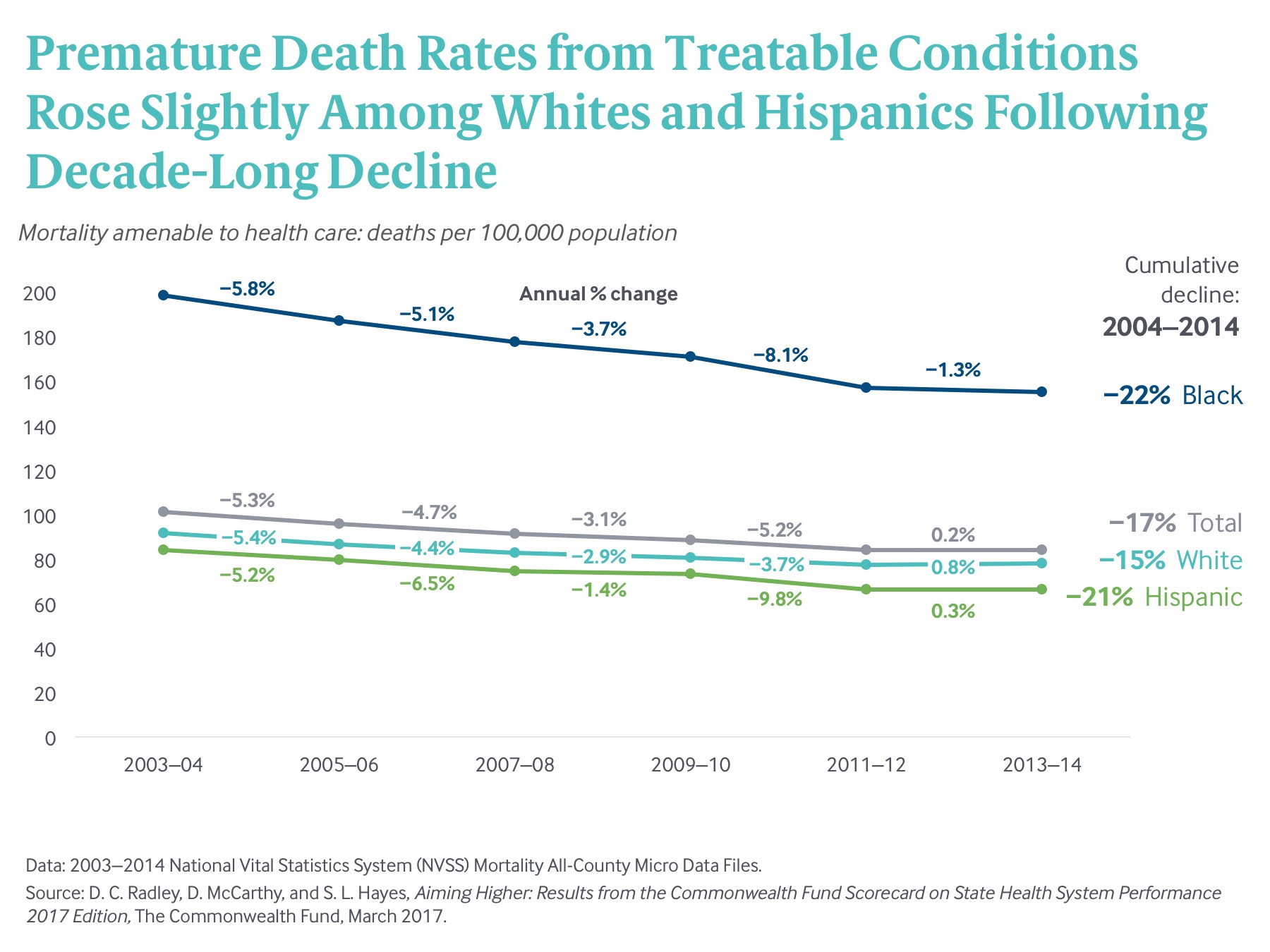
Taking a closer look at deaths before age 75 that might have been prevented with accessible and effective health care, we find a decade-long decrease in mortality reversed course in recent years as the rate rose slightly between 2011–12 and 2013–14 (Exhibit 8). There is also a significant racial disparity in premature death rates. Over the last decade, African Americans experienced a greater reduction in mortality amenable to health care than did other racial or ethnic groups.
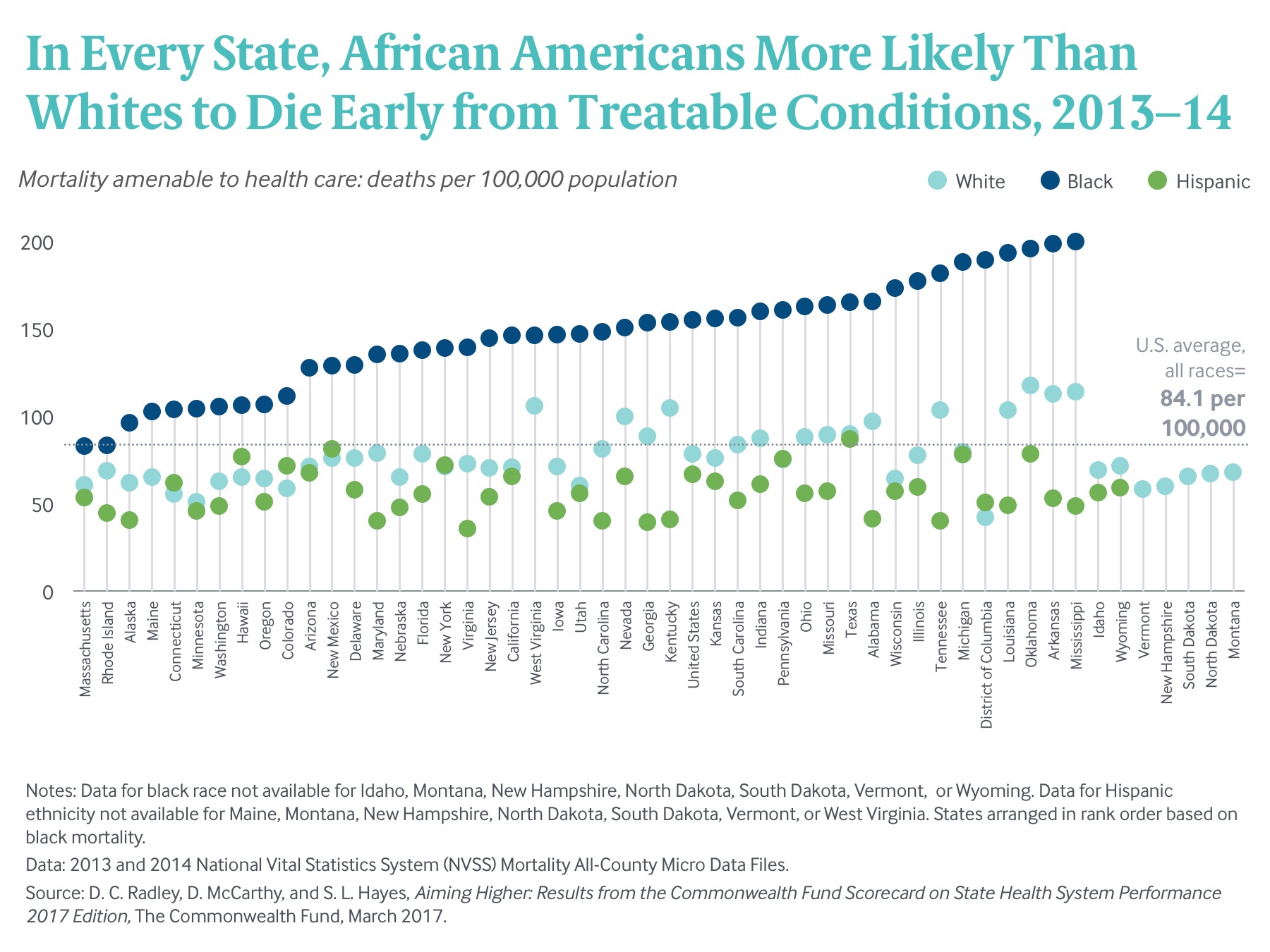
However, that reduction did not eliminate disparities for African Americans, who in all states (where data were available) remained more likely than whites or Hispanics to die before age 75 from treatable conditions in 2013–14. In 10 states and the District of Columbia, there was a more than twofold disparity in rates between blacks and both whites or Hispanics (Exhibit 9).
While these overarching trends in mortality are concerning, there is some good news. Deaths from breast and colon cancer fell between 2012 and 2014, as did adult smoking rates, a key risk factor for heart disease and lung cancer. The positive health effects likely to accrue from reduced rates of smoking may be outweighed, however, by the negative health effects of obesity (Appendix F2). (notes) S. T. Stewart, D. M. Cutler, and A. B. Rosen, “Forecasting the Effects of Obesity and Smoking on U.S. Life Expectancy,” New England Journal of Medicine, Dec. 3, 2009 361(23):2252–60.
The health care coverage and access gains noted earlier promote more regular access to primary care, which has been linked to earlier disease detection and greater adherence to treatment regimens, among other benefits. (notes) K. Davis, M. K. Abrams, and K. Stremikis, “How the Affordable Care Act Will Strengthen the Nation’s Primary Care Foundation,” Journal of General Internal Medicine, published online April 27, 2011. But strengthening primary care is not enough. The social and other determinants of health must also be addressed to produce hoped-for gains in health outcomes.
Threefold Variations Across Measures Between Top- And Bottom-Performing States
The Scorecard is a stark reminder that where you live affects your ability to access high-quality health care and your prospects for a healthy life. On average, performance in the highest-ranked state on a given indicator was three times better than in the lowest-ranked state, with even wider variation for some indicators. For example, there was an almost sixfold difference in uninsured rates among working-age adults (23% in Texas vs. 4% in Massachusetts) and a fourfold difference in rates of readmissions to the hospital among Medicare beneficiaries (10 per 1,000 in Hawaii vs. at least 40 per 1,000 in the District of Columbia, Maryland, Mississippi, and New Jersey).
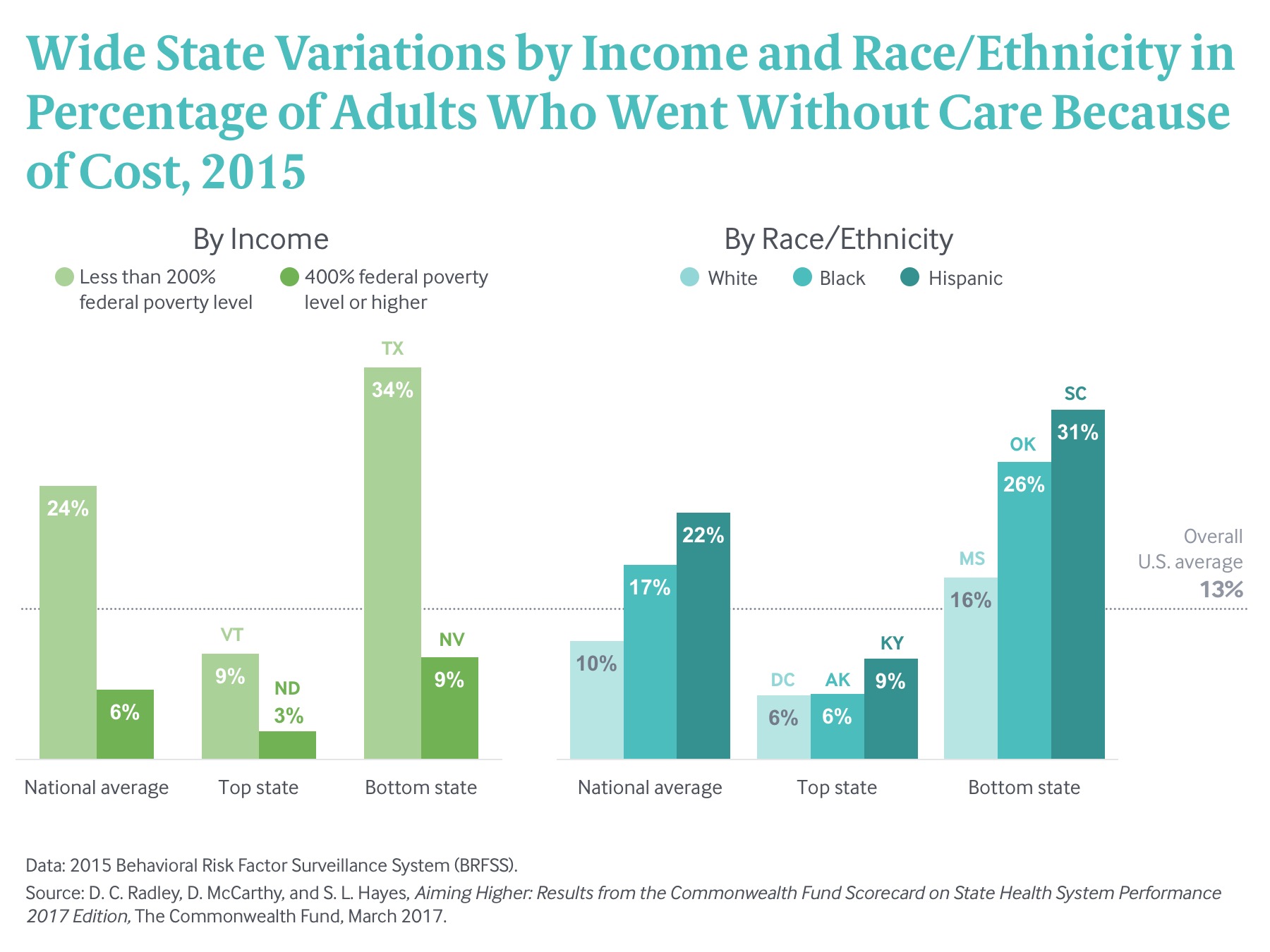
The Scorecard also finds continuing disparities for those with low incomes and for members of racial and ethnic minority groups in most—but not all—states compared to national norms. For example, the share of low-income adults who skipped needed care because of cost was 21 percentage points higher than the overall U.S. average in Texas (34% vs. 13%), whereas it was four points lower than the overall U.S. average in Vermont (9%) (Exhibit 10). Similarly, rates of forgone care due to cost for racial and ethnic minority populations are much higher than the overall U.S. average in the worst-performing states: Oklahoma had the highest rate for blacks and South Carolina had the highest rate for Hispanics. Despite these disparities, recent trends are promising. As state performance improved overall for many indicators, state equity gaps also more often narrowed than widened for the majority of equity indicators tracked by the Scorecard. (Appendix G2).
Health care inequities result from disparities in access to and availability of care (e.g., the number of people who have insurance or who visit a dentist regularly), health outcomes (e.g., mortality), and risks (e.g., the number of people who are obese or are smokers) between various groups.
The Scorecard’s Equity dimension looks at two vulnerable populations: low-income people and those who belong to racial and ethnic minorities. A state’s performance is based on gaps in equity—that is, the difference between the state’s vulnerable population and the U.S. average for any given indicator. Improvement is defined as an improvement in the state’s vulnerable group rate and a narrowing in the performance gap between the vulnerable group and the U.S. average.
Across the nation, health care equity remains an unfulfilled goal. The health insurance expansions brought about by the Affordable Care Act (assuming they are not reversed) offer the opportunity to close these gaps.
-
20 million more adults and children insured, beyond those who already gained coverage through the ACA
-
14 million fewer adults skipping care because of its cost
-
26 million more adults with a usual source of care
-
12 million more adults receiving recommended cancer screenings
-
513,000 more young children receiving all recommended vaccines
-
1 million fewer Medicare beneficiaries receiving a high-risk prescription drug
-
124,000 fewer hospital readmissions among Medicare beneficiaries ages 65 and older
-
1.4 million fewer emergency room visits for nonemergency care or conditions treatable with primary care
-
90,000 fewer deaths before age 75 from treatable diseases
Implications
All states have the opportunity to improve, including those at the top. On certain indicators, states that ranked lower overall performed better than those at the top of the overall rankings, which suggests that states can learn from each other. If every state achieved the performance of the top-ranked state on each Scorecard indicator, their residents and the country as a whole would realize dramatic gains in access, quality, efficiency, and health outcomes (Exhibit 11).
States can take various steps to promote improvement. Examples include using value-based purchasing, establishing rules to ensure equitable access and competitive insurance markets, setting strategies for health information technology and exchange, and supporting public health and community-based organizations that address social determinants of health. Health systems with a stronger primary care orientation generally achieve better outcomes. (notes) B. Starfield, L. Shi, and J. Macinko, “Contribution of Primary Care to Health Systems and Health,” Milbank Quarterly, 2005 83(3):457–502; M. W. Friedberg, P. S. Hussey, and E. C. Schneider, “Primary Care: A Critical Review of the Evidence On Quality and Costs of Health Care,” Health Affairs, May 2010 29(5):766–72. Promoting an adequate primary care workforce, especially in underserved areas, may require collaborating with other payers to support the development of effective primary care medical homes, among other actions.
States have unequal economic circumstances and resources to support improvement. The gains brought about by Medicaid expansion and marketplace subsidies in places like Kentucky highlight the role the federal government can play in helping to equalize opportunity. Efforts in California and elsewhere show how states can leverage federal reforms to achieve their own goals. These gains may be challenged by the proposed repeal and replacement of the Affordable Care Act, which could lead to widening inequality between and within states.
With the future uncertain, it will be more important than ever to track state health system performance as states assume greater responsibility for the future of health policy.
